A recent study from researchers in China has uncovered significant imbalances in specific immune cell populations circulating in individuals living with primary Sjögren’s syndrome. These findings suggest the cellular alterations could be more than just symptoms; they may actively drive the progression of the autoimmune condition and influence how severe it becomes.
This exploration into the immune system’s role offers vital insights. “Our study demonstrates significant alterations in circulating immune cell populations in patients with [primary Sjögren’s], linking these changes to clinical disease activity,” the research team stated. Understanding these shifts is crucial because autoimmune diseases like Sjögren’s happen when the body’s immune system mistakenly attacks its own tissues, leading to inflammation. In Sjögren’s, this often targets moisture-producing glands, causing hallmark symptoms like dry eyes and dry mouth.
Critically, the scientists highlighted three particular types of immune cells. These could potentially serve as biological markers to track disease activity or even become targets for developing novel, targeted therapies in the future. As the researchers put it, “These findings may provide mechanistic insights into … pathogenesis [disease development] and establish a foundation for developing … targeted therapeutic strategies.” The full findings were published in the International Journal of Rheumatic Diseases.
Understanding Primary Sjögren’s Syndrome
Primary Sjögren’s syndrome occurs when the autoimmune condition exists independently, without another underlying autoimmune disease. It is a chronic, systemic disorder characterized by immune-mediated damage, particularly to the lacrimal and salivary glands. However, systemic involvement affecting various organs is also common.
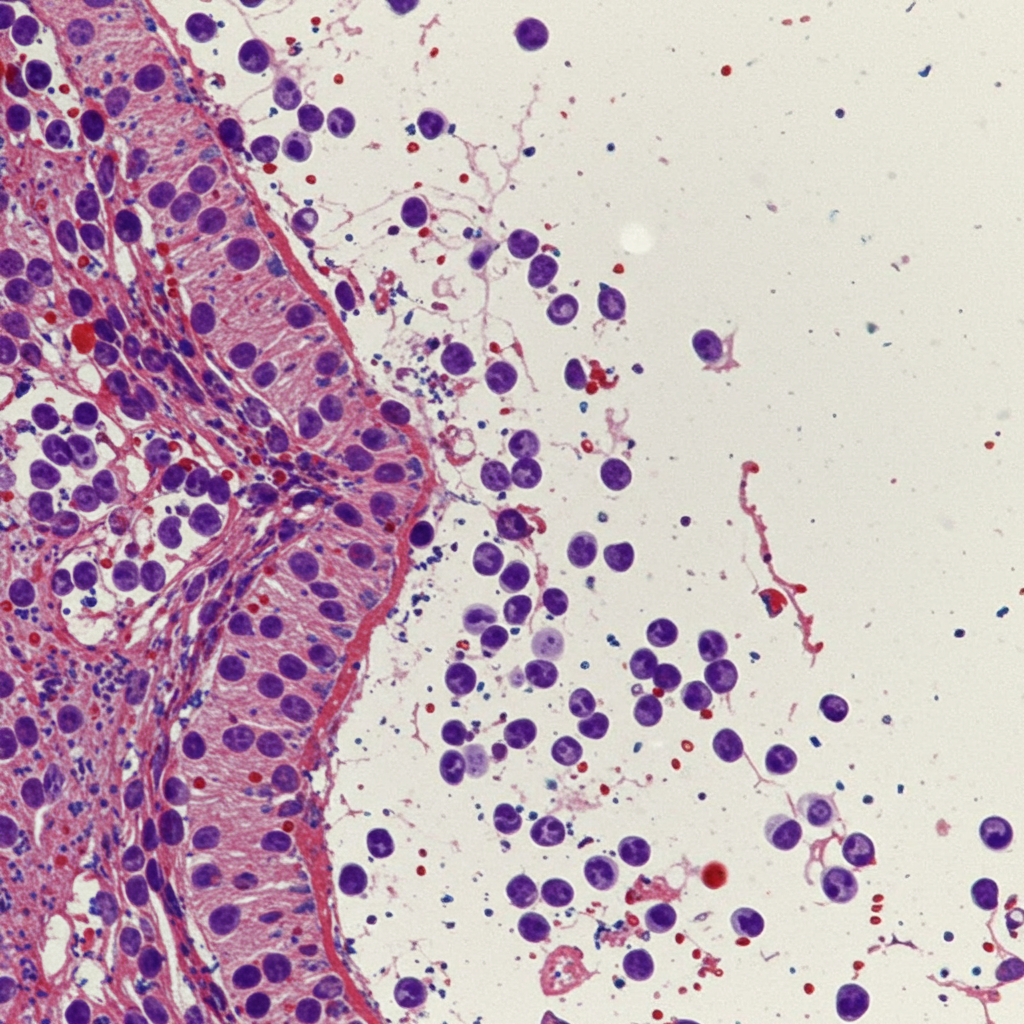
The pathogenesis is complex, involving genetic susceptibility (certain HLA genes play a role), environmental triggers like viral infections (Epstein-Barr virus is often cited), and a breakdown of immune tolerance. This leads to autoreactive T and B cells targeting the body’s own components. These immune cells don’t just cause damage in specific tissues; they also circulate throughout the bloodstream. The current study focused on changes seen in these circulating immune cells, specifically lymphocytes, a type of white blood cell.
Circulating Immune Cell Patterns Identified
The researchers aimed to clarify the relationship between these peripheral immune cell alterations and clinical outcomes in primary Sjögren’s. They analyzed blood samples from 43 individuals with primary Sjögren’s and compared them to a control group of 46 people without chronic inflammatory disorders, matched for age and sex.
Overall levels of B cells, which are responsible for producing antibodies, were notably higher in the Sjögren’s patient group compared to controls. A specific subtype, known as CD21-/low B-cells, was particularly elevated. This subtype is also frequently found at high levels in other chronic immune conditions. The study revealed a significant correlation: higher levels of these CD21-/low B-cells were associated with greater disease severity in the Sjögren’s population studied. Interestingly, other subtypes of B cells showed lower levels in the Sjögren’s patients than in the control group, indicating a complex pattern of B cell dysregulation.
“Our findings demonstrate profound alterations in peripheral lymphocyte subsets in patients with [primary Sjögren’s], revealing distinct immune dysregulation patterns within T and B cell populations,” the research team emphasized. These changes included some immune cell subtypes being significantly more abundant and others significantly less abundant. For several subtypes, the observed levels correlated with disease severity scores, as measured using the EULAR Sjögren’s Syndrome Disease Activity Index (ESSDAI), a standardized tool for assessing disease activity.
Specific T Cell Alterations Uncovered
While the total numbers of certain T cells, such as T-helper (Th) and T-follicular helper (Tfh) cells, appeared similar between the Sjögren’s patients and controls, a closer look at T cell subtypes revealed important distinctions.
Significantly, two specific types of helper T cells – Th2 and Th17 cells – were found to be notably increased in the Sjögren’s group. Helper T cells like Th2 and Th17 play critical roles in coordinating immune responses. Elevated Th17 cells, in particular, are known to contribute to B cell hyperactivity and inflammation in glands, supporting their potential involvement in the early stages of Sjögren’s development. Research indicates that an imbalance, often favoring pro-inflammatory Th17 cells over regulatory T cells, is key in Sjögren’s gland pathology. These cells contribute to inflammatory processes partly by releasing cytokines that affect glandular tissues.
Furthermore, the study found that the total count of cytotoxic T (Tc) cells was significantly higher in patients with Sjögren’s. Cytotoxic T cells are typically involved in targeting and eliminating damaged or infected cells. The data showed that elevated levels of total Tc cells were also linked to more severe disease scores (ESSDAI). Conversely, two specific subtypes of cytotoxic T cells, Tc1 and Tc17, were found to be significantly decreased in Sjögren’s patients compared to the control group. The researchers noted that higher levels of Tc1 cells were associated with milder disease severity.
Implications for Understanding and Treating Sjögren’s
These detailed findings about circulating immune cell populations and their link to disease severity provide valuable clues into the underlying processes driving primary Sjögren’s syndrome.
The researchers highlighted the importance of their discoveries: “The identification of CD21−/low B cells as potential mediators of disease activity, alongside Th17 or Tc cell imbalances, highlights actionable pathways for further exploration.” This suggests that targeting these specific cell types or the pathways regulating them could be a promising strategy. The identified cells could also serve as valuable biological markers, potentially helping clinicians assess disease state and progression.
The broader field of autoimmune disease research is increasingly focused on targeted therapies that selectively modulate specific immune cell populations or pathways, rather than using broad immunosuppression. Approaches like specific antibody therapies, which can target particular cell surface markers or cytokines (like BAFF, which promotes B cell survival and is often elevated in Sjögren’s), or therapies that interfere with specific signaling pathways (like JAK-STAT, involved in cytokine signaling), are areas of active investigation for autoimmune conditions. While antigen-specific immunotherapies aiming to restore tolerance are also emerging, understanding the precise cellular dysregulation in diseases like Sjögren’s is a necessary first step to develop such targeted interventions.
However, the scientists also included important caveats. They noted that the patient population in this specific study tended to have milder forms of Sjögren’s. It is possible that individuals with more severe manifestations of the disease might exhibit different patterns of immune dysregulation. This could imply that distinct immune processes might be involved depending on the disease stage or severity, a concept supported by research showing differences in tissue pathology and immune cell activity between different forms or stages of Sjögren’s. Therefore, they recommend larger, multicenter studies with more diverse patient groups to confirm these observations and fully explore their potential implications for treatment development.
Frequently Asked Questions
What specific immune cell types were found dysregulated in this Sjögren’s study?
The study identified several circulating immune cell types that were imbalanced in people with primary Sjögren’s syndrome compared to healthy individuals. Key findings included higher overall levels of B cells, particularly an increase in CD21-/low B-cells. Regarding T cells, the study found altered subtype levels, specifically increased levels of Th2 and Th17 helper T cells, and higher total cytotoxic T cells. Some of these altered cell levels, such as CD21-/low B-cells and total cytotoxic T cells, correlated with greater disease severity.
Where can I find more information about studies like this on Sjögren’s syndrome?
This specific study, titled “Immunophenotypic Profiling Reveals Circulating Lymphocyte Dysregulation in Primary Sjögren’s Syndrome,” was published in the International Journal of Rheumatic Diseases. Researchers focusing on rheumatology, immunology, and oral health frequently publish studies on Sjögren’s syndrome in various medical and scientific journals. Searching databases like PubMed or Google Scholar using keywords like “Sjögren’s syndrome,” “immune cells,” “lymphocytes,” “autoimmunity,” and “pathogenesis” can help locate relevant research articles in these publications.
How do these findings about immune cells impact potential treatments for primary Sjögren’s?
The discovery of specific immune cell types that are dysregulated and linked to disease severity in primary Sjögren’s syndrome is significant for future treatment development. These identified cells, such as CD21-/low B-cells, Th17 cells, and cytotoxic T cells, represent potential targets for new therapies. Instead of broadly suppressing the immune system, future treatments might aim to specifically modulate the activity or levels of these particular cell types or the molecular pathways they utilize (like cytokine signaling pathways). These findings could also lead to the development of biomarkers, allowing doctors to potentially use blood tests to better monitor disease activity and response to treatment.