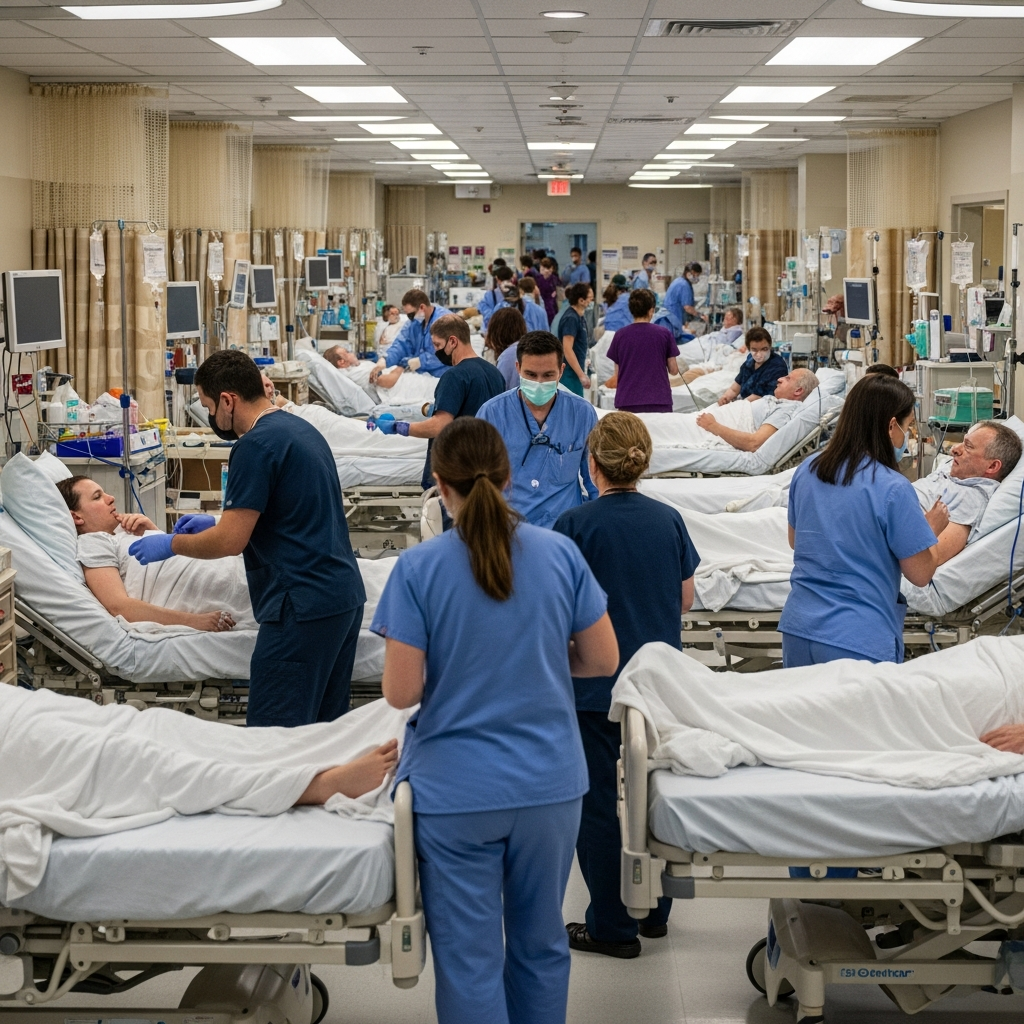
Utah health officials are issuing a stark warning about a widespread measles outbreak that has shocked medical professionals and patients alike. Described as “worse than expected,” this highly contagious viral infection is causing severe complications, pushing hundreds into emergency rooms and dozens into hospital care, including intensive care units. This critical public health crisis underscores the urgent need for vaccination, particularly as the outbreak continues to expand across the state and mirrors a concerning national resurgence of measles cases. Understanding the true severity and spread of the Utah measles outbreak is vital for community safety.
The Alarming Reality: Measles Cases Prove Unexpectedly Severe
For many Utah residents and even seasoned medical staff, the current measles outbreak has revealed a shocking truth: measles is far from a mild childhood illness. Dr. Leisha Nolen, Utah’s state epidemiologist, emphasizes that this is a “severe illness,” not a “mild infection.” Patients and their caregivers have consistently reported that the disease is “so much worse than what they expected.” This sentiment highlights a critical gap in public perception, as many expressed regret, wishing they had vaccinated themselves or their children if they had understood the true extent of the illness.
The medical community, many of whom have not encountered measles in their careers until recently, is equally surprised. Nurse practitioner Amanda Jocelyn, practicing in southern Utah, shared her shock at the extreme illness and prolonged recovery times among her patients. She noted that children become “very, very ill,” with parents and caregivers frequently falling sick alongside them. This unprecedented severity is prompting health authorities to push for immediate preventive action.
Unforeseen Complications Beyond the Typical Rash
The gravity of the current Utah measles outbreak is not just in the number of cases, but in the serious health complications emerging. Medical reports indicate that more than 120 individuals have sought emergency care, with 31 requiring at least one night of hospitalization. Alarmingly, three patients have been admitted to intensive care units (ICU), a clear indicator of the virus’s severe impact.
Specific severe cases illustrate the unexpected dangers. One patient experienced an aplastic crisis, a life-threatening condition where bone marrow ceases red blood cell production, leading to severe anemia. Another, an otherwise healthy young mother, developed measles-induced hepatitis, a severe liver inflammation that also necessitated an ICU stay. These complications underscore that measles can affect even robust individuals profoundly, not just those with compromised immune systems. High fevers, often reaching 105°F for a week, severe coughing, and pneumonia requiring oxygen support are also commonly observed.
Tracking the Spread: A Timeline of the Utah Measles Outbreak
The measles outbreak in Utah first began in June of the previous year (2025), but it significantly escalated in August. Initially, the virus was concentrated in a tight-knit community in southwestern Utah, bordering Arizona, largely linked to former members of the Fundamentalist Church of Jesus Christ of Latter-day Saints (FLDS). This initial cluster saw 203 infections in the southwest Utah health district alone.
However, the outbreak has since expanded its reach. The virus has moved northward, affecting areas in and around Salt Lake City. Large school athletic events, particularly state wrestling tournaments held in January and February, have been identified as key spreading points. The TriCounty Health Department, covering three counties in the northeastern part of the state, recently reported five new cases connected to a state wrestling tournament, highlighting the potential for delayed symptom onset, which can take up to 21 days post-exposure. Other significantly impacted areas include Utah County (50 cases) and Salt Lake County (44 cases). As of March 7, 2026, Utah has recorded 358 measles cases since the outbreak began.
A National Resurgence: Measles on the Rise Across the U.S.
The situation in Utah is not isolated but reflects a disturbing national trend. The Centers for Disease Control and Prevention (CDC) reported 1,281 measles cases across the U.S. since January 1, 2026. This number already exceeds half of the total 2,283 cases reported in the entire previous year (2025), which was the highest number in over 30 years. Thirty states have reported outbreaks this year, indicating a widespread resurgence of this preventable disease.
The vast majority of these national cases, 93%, are occurring in unvaccinated individuals. Children and teenagers are disproportionately affected, with 23% of cases in children younger than 5 years old and 54% in those aged 5 through 19. This demographic pattern aligns with concerns about declining MMR vaccination rates among kindergarteners, which fell below the critical 95% herd immunity threshold.
Lessons from South Carolina: Vaccination Drives Down Cases
In South Carolina, which experienced the nation’s largest measles outbreak in a generation, there’s a glimmer of hope. Cases are finally slowing, with only six new infections reported last week, bringing their total to 991. Dr. Linda Bell, South Carolina’s state epidemiologist, attributes this positive shift to increased vaccination efforts among residents.
In Spartanburg County, the epicenter of South Carolina’s outbreak, measles vaccinations surged by an impressive 70% in February compared to the same period last year. The state also administered over 4,800 MMR doses to infants aged 6-11 months. This success story underscores the direct impact that increased immunization can have on containing and eventually ending large-scale outbreaks, though vigilance remains crucial, especially with events like spring break approaching. The CDC is even deploying epidemic intelligence officers to South Carolina to study the outbreak’s spread.
Vaccination: The Most Potent Defense Against Measles
The MMR vaccine (measles-mumps-rubella) remains the gold standard for protection against measles. Two doses provide 97% protection against infection, a defense that typically lasts a lifetime. Despite claims about vaccine imperfections, this efficacy rate is remarkably high and represents the most effective public health tool we have. While Utah’s state vaccination rate against measles is approximately 90%, most of the confirmed cases are among the unvaccinated. Even among those who contracted measles, around 8-10% had at least one dose, but typically experienced milder symptoms.
During active outbreaks like the one in Utah, there’s a crucial adjustment to vaccination advice for infants. While typically administered around one year of age, babies as young as 6 to 11 months can now receive an early, extra shot. This recommendation is vital because young children are particularly vulnerable to serious complications, such as pneumonia, which is the leading cause of death for children under 5 who contract measles. The second dose can also be given just one month after the first, rather than waiting until age four.
Recognizing Measles Symptoms and Understanding Contagion
Knowing the symptoms of measles is crucial for early detection and preventing further spread. Measles typically begins with flu-like symptoms that can easily be mistaken for a common cold or other respiratory illness. These initial signs include:
High fever, often reaching 103°F to 105°F and lasting up to a week.
Persistent, severe cough.
Runny nose.
Headache.
Within a few days, patients often develop red, watery eyes and tiny white spots (known as Koplik spots) inside the mouth. This phase is highly contagious, occurring up to four days before the telltale splotchy red rash appears. The characteristic rash typically starts on the scalp and neck, then spreads across the trunk, arms, and legs.
Measles is one of the most contagious infectious diseases known, airborne and capable of lingering in the air for several hours. This means individuals can contract the virus simply by walking through a space where an infected person has recently been, making rapid spread at public gatherings like school events particularly concerning.
Protecting Vulnerable Populations: A Critical Priority
The ongoing measles outbreak poses significant risks to several vulnerable groups. Infants, especially those too young to be fully vaccinated, face serious complications. The adjusted vaccination age for babies 6 months and older aims to offer earlier protection. Immunocompromised individuals also face elevated risks and cannot always receive the vaccine.
Pregnant women represent another extremely vulnerable group. The measles vaccine cannot be administered during pregnancy. If a pregnant woman contracts measles, there is a “fairly high risk” of pregnancy loss. Furthermore, if the infection occurs shortly before delivery, the baby can contract measles, leading to poor outcomes for newborns, including potential brain damage from high fevers. Therefore, women hoping to become pregnant are strongly advised to ensure they are vaccinated against measles beforehand. Caregivers of sick individuals also frequently contract the illness, highlighting the virus’s high transmissibility.
Taking Action: What Utah Residents Need to Do
In light of the severe and expanding Utah measles outbreak, public health officials are urging proactive steps. For those who are unvaccinated or partially vaccinated, getting the MMR vaccine immediately is the most effective form of protection.
If you suspect exposure to measles or begin to develop symptoms, it is critical to stay home for 21 days to prevent further spread. Contact your healthcare provider immediately, but be sure to call ahead before visiting any clinic or emergency room. This allows medical staff to take necessary precautions to protect other patients and prevent the virus from spreading within healthcare settings. Avoiding public spaces and vulnerable populations (such as young children, the elderly, and pregnant women) is paramount if you have been exposed or are experiencing symptoms. While individuals maintain the right to choose regarding vaccination, health officials emphasize that informed decision-making based on the current, severe reality of measles is crucial for public health.
Frequently Asked Questions
What makes the current Utah measles outbreak so severe compared to previous years?
The current Utah measles outbreak, which began in June 2025 and escalated through early 2026, is described as “worse than expected” due to the high incidence of severe complications. Unlike previous low case counts for decades, this outbreak has led to over 120 emergency room visits, 31 hospitalizations, and three intensive care unit admissions. Patients have experienced life-threatening conditions like aplastic crisis (bone marrow shutdown causing anemia) and measles-induced hepatitis (severe liver inflammation), even in otherwise healthy individuals. Health officials and medical professionals, many encountering measles for the first time, are shocked by the intensity and prolonged recovery periods, underscoring that this is a truly “severe illness.”
Where has the measles outbreak spread within Utah, and which communities are most affected?
The measles outbreak in Utah initially concentrated in southwestern Utah, specifically within a tight-knit community bordering Arizona, largely linked to former members of the Fundamentalist Church of Jesus Christ of Latter-day Saints (FLDS). This region accounted for 203 of the total 358 cases. The virus has since spread north, affecting areas around Salt Lake City, with significant transmission linked to large school athletic events, such as state wrestling tournaments. Other heavily impacted areas include Utah County (50 cases) and Salt Lake County (44 cases), with recent cases also reported in the TriCounty Health Department area in northeastern Utah, further demonstrating its expansion across the state.
Who should get the MMR vaccine immediately, especially given the ongoing Utah measles outbreak?
Given the ongoing and severe Utah measles outbreak, individuals who are unvaccinated or partially vaccinated against measles should get the MMR vaccine immediately. This includes adults who are unsure of their vaccination status, as well as children. Specifically, due to the outbreak’s severity and the vulnerability of infants, babies as young as 6 to 11 months old can now receive an early, additional MMR shot. Pregnant women cannot receive the vaccine, so those planning pregnancy are strongly advised to get vaccinated beforehand. Anyone in close contact with confirmed cases or in affected areas should also prioritize vaccination.
—