South Carolina is at the forefront of a worrying measles resurgence, grappling with an outbreak that has contributed significantly to a nationwide surge in cases. This highly infectious disease, once nearly eliminated in the U.S., now poses a critical public health challenge. Understanding the current measles situation in South Carolina and its broader implications for community health is essential for residents and healthcare providers alike. This comprehensive guide delves into the details of the outbreak, its causes, the wider national context, and the vital role of vaccination in protecting public health.
The Alarming Rise: South Carolina at the Epicenter
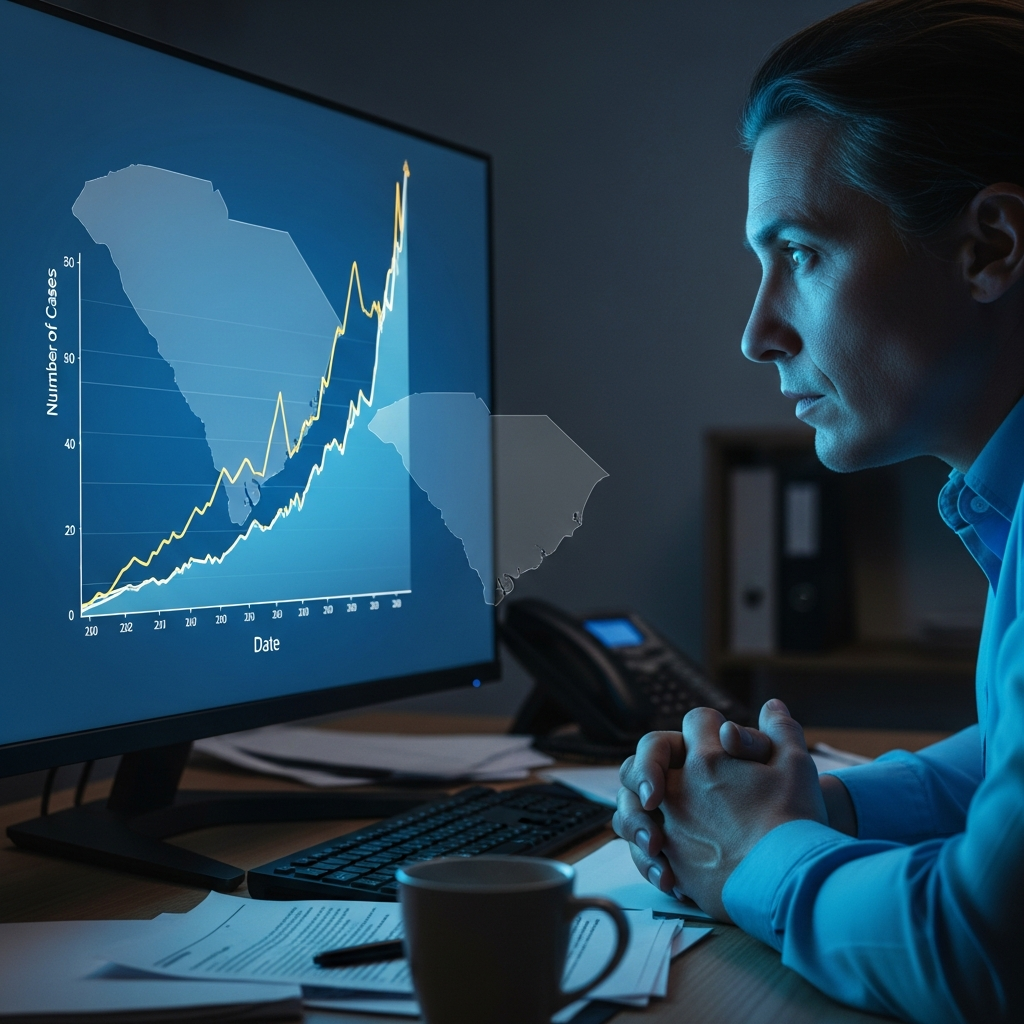
The Palmetto State finds itself in a critical position as a significant driver of the current measles crisis. With 129 confirmed cases in South Carolina alone, this outbreak has fueled the most substantial measles resurgence the United States has seen in a quarter-century. This localized surge highlights the vulnerability of communities with lower vaccination rates, creating fertile ground for the highly contagious virus to spread rapidly. Public health officials are sounding the alarm, emphasizing the severe implications for both individual health and the healthcare system. The financial burden is also immense, with outbreak-related costs averaging an estimated $43,000 per case nationally.
A National Crisis: America’s Measles Elimination at Risk
The situation in South Carolina mirrors a troubling national trend. As of December 2025, the U.S. recorded a staggering 1,912 confirmed measles cases, marking the highest count since the disease was declared eliminated in the year 2000. This dramatic increase has led to three measles-related deaths in 2025. Experts from Johns Hopkins Bloomberg School of Public Health warn that the nation’s measles elimination status is now gravely at risk. Elimination is defined by the absence of continuous transmission for 12 months or more. If continuous transmission can be demonstrated from January 2025 through January 2026, the U.S. could officially lose this critical public health achievement. The Americas region already forfeited its elimination status in November 2025. Investigations into specific D8 genotype strains are ongoing, requiring sophisticated genomic sequencing to definitively link outbreaks.
Unpacking the “Why”: Gaps in Immunity and Vaccine Hesitancy
A stark statistic underscores the primary reason for this resurgence: an overwhelming 92% of measles cases in 2025 occurred in unvaccinated individuals or those with unknown vaccination status. This clearly points to long-standing undervaccination in certain communities as a key factor. Surprisingly, the age distribution of cases shows roughly 25% in children under five and 33% in adults over 20, deviating from typical patterns. For those unsure of their immunity status, healthcare professionals recommend revaccination rather than routine antibody testing, ensuring robust protection. This proactive approach helps close immunity gaps that the virus readily exploits.
Beyond Measles: A Complex Public Health Landscape
The measles outbreak is not an isolated incident. It unfolds amidst a challenging broader public health environment. The nation is also battling a difficult respiratory virus season, marked by the emergence of a new H3N2 influenza variant, designated clade K. This variant carries mutations that may help it evade some vaccine-induced protection, potentially leading to more severe flu seasons. Simultaneously, overall vaccination rates for both influenza and COVID-19 have seen a “modest but consistent” decline across all age groups since the pandemic’s acute phase. This reduction is partly due to a diminished public health “push.” Compounding these issues are concerns regarding federal health communication. Experts criticize limited public briefings on outbreaks and mixed messages from leadership, which can sow doubt and lead to inaction, even among those not inherently anti-vaccine.
The Enduring Power of Vaccines: A Historical Perspective
Vaccines stand as one of humanity’s greatest public health achievements. Their history dates back centuries, with early inoculation techniques in ancient China, Africa, and Turkey. In the U.S., Cotton Mather promoted smallpox vaccination in 1721. Edward Jenner’s groundbreaking cowpox vaccine in 1796 paved the way for modern immunology and eventually the global eradication of smallpox. Massachusetts led the charge in the U.S., enacting the first state law mandating vaccinations for schoolchildren in 1855. By 1970, 29 states had similar mandates. The U.S. Supreme Court has repeatedly upheld the legality of mandatory vaccination, notably in Jacobson v. Massachusetts (1905). The highly effective Salk polio vaccine, developed in 1955, contributed to the elimination of polio in the U.S. by 1979. These historical milestones underscore vaccines’ profound impact on preventing widespread illness and death.
Debunking Misinformation: Addressing Vaccine Concerns
Despite overwhelming scientific consensus, vaccine hesitancy persists, often fueled by debunked claims. The most prominent example is Andrew Wakefield’s fraudulent 1998 Lancet article, which falsely linked the MMR vaccine to autism. This article was retracted in 2010, and Wakefield lost his medical license. Similarly, concerns about thimerosal, a mercury-based preservative, were widely investigated, with scientific studies consistently finding no causal link between vaccines (including MMR and thimerosal-containing vaccines) and autism. Yet, these discredited claims continue to influence public opinion. A 2024 Gallup poll revealed a significant decline in the perception of childhood vaccines’ importance, dropping from 64% in 2001 to just 40% of Americans considering them “extremely important.” This shift in perception poses a serious threat to community immunity.
The Case for Community Protection: Why Mandates Matter
Vaccine mandates, particularly for school entry, are crucial tools for maintaining public health. While no federal laws enforce vaccination, all 50 states require specific immunizations for public school attendance, usually with medical or religious exemptions. The benefits of these mandates are clear:
Necessity: Vaccine-preventable diseases remain a threat. The 1,912 measles cases in the U.S. in 2025, a sharp increase from 285 in 2024, demonstrate their continued presence. Many diseases are “only a plane ride away,” making imported cases a constant concern. Measles vaccines alone have prevented an estimated 93-97 million deaths globally between 1974 and 2024.
Herd Immunity: Mandates ensure high population immunity, creating a protective shield for vulnerable individuals who cannot be vaccinated (e.g., infants, immunocompromised individuals). Outbreaks frequently occur when herd immunity thresholds are not met, allowing diseases to spread unchecked.
- Cost Savings: Preventing illness through vaccination is far more cost-effective than treating diseases. Measles, for instance, can incur public health costs averaging $47,962 per case in some states. Overall, vaccinated children born between 1994 and 2018 have generated an estimated $406 billion in direct cost savings and $1.9 trillion in societal cost savings.
- conexiant.com
- www.britannica.com
It’s also important to distinguish between disease elimination (not present in a region) and eradication (not globally existent). Diseases like polio and measles were eliminated in the U.S. due in large part to widespread vaccination.
Navigating Personal Choice and Public Safety
While proponents emphasize public health, opponents of vaccine mandates often cite constitutional rights, advocate for counseling over mandates, and argue against government interference in personal medical choices. These perspectives highlight the ongoing tension between individual liberty and collective well-being. However, declining vaccination rates can have tangible consequences for families. Unvaccinated children may face school suspensions and quarantines, as seen in various outbreaks. Some pediatricians may refuse to treat unvaccinated children, and in extreme cases, legal experts have suggested potential criminal prosecution for parents whose unvaccinated children infect and harm others.
Recent developments further complicate the landscape. A hypothetical scenario for 2025-2026 suggests significant shifts under a new administration, with the CDC reportedly removing six vaccines (Hepatitis A, Hepatitis B, influenza, meningitis, RSV, and rotavirus) from the recommended childhood schedule, citing “transparency and informed consent.” Experts widely disagree with such abrupt changes, calling them “alarming, unnecessary, and will endanger the health of children.” Eleven vaccines, including MMR, DTaP, Hib, pneumonia, IPV, varicella, and HPV, would remain on the recommended schedule.
Global Threats, Local Vigilance: Protecting Our Borders
The U.S. measles resurgence cannot be viewed in isolation. Globally, a “perfect storm” is brewing for vaccine-preventable diseases. Declining vaccine coverage worldwide, loosening school entry requirements, and, critically, U.S. funding cuts to key global health organizations like USAID, GAVI, and the WHO are projected to lead to more frequent and larger outbreaks internationally. This, in turn, significantly increases the likelihood of pathogen importations into the United States, posing a continuous threat to our domestic public health. To counter this, the International Vaccine Access Center (IVAC) has launched a measles tracker, providing crucial county-level outbreak data that fills gaps in official reporting, helping communities stay informed and vigilant.
Frequently Asked Questions
What is causing the recent surge in measles cases across the U.S.?
The significant surge in U.S. measles cases, reaching a 25-year high with over 1,900 confirmed cases in 2025, is primarily driven by declining vaccination rates in various communities. An overwhelming 92% of these cases occurred in individuals who were either unvaccinated or whose vaccination status was unknown. This creates pockets of vulnerability where the highly contagious virus can rapidly spread. Outbreaks, such as the 129 cases in South Carolina, contribute substantially to the national increase, threatening the nation’s measles elimination status.
Should adults consider revaccination for measles if unsure of their immunity?
Yes, if you are an adult unsure of your measles immunity, public health experts highly recommend revaccination. The measles resurgence has shown an unexpected age distribution, with a significant percentage of cases occurring in adults over 20 due to long-standing undervaccination or waning immunity. Rather than undergoing routine antibody testing, which can be less conclusive, a booster dose of the MMR (Measles, Mumps, Rubella) vaccine is a safe and effective way to ensure robust protection against the virus. Consult your healthcare provider for personalized advice.
Where can I find reliable information on measles outbreaks and vaccination guidelines?
For reliable information on measles outbreaks and vaccination guidelines, several authoritative sources are available. The Centers for Disease Control and Prevention (CDC) website (cdc.gov) provides official recommendations, statistics, and educational materials. Additionally, the International Vaccine Access Center (IVAC) has launched a measles tracker, which offers county-level outbreak data to help communities monitor local situations. Your local or state public health department websites are also excellent resources for region-specific information and vaccination clinics. Always refer to established medical and public health organizations for accurate, evidence-based guidance.
Conclusion
The measles outbreak in South Carolina is a stark reminder of the fragile nature of public health achievements and the critical importance of sustained vigilance. The resurgence of measles across the U.S., driven by declining vaccination rates and exacerbated by broader public health challenges, underscores the need for collective action. Understanding the science behind vaccines, dispelling misinformation, and upholding strong public health policies like school mandates are paramount. By prioritizing robust immunization efforts and fostering clear, consistent health communication, we can protect our communities, preserve our elimination status, and safeguard the well-being of future generations against preventable diseases. Staying informed and consulting with healthcare professionals remains the best defense for every individual and family.